 Your new post is loading...
 Your new post is loading...
Introduction When it comes to our muscles, many of us often don’t stretch each muscle group at least two to three times per week. From waking up in the morning, we stretch our arms, legs, and back to relieve any stiffness or soreness from the previous day. However, many individuals deal with musculoskeletal issues that can affect not only the back and the neck but also the upper and lower extremities of the body, causing pain-like symptoms that can worsen throughout the entire day if not treated right away. When this happens, musculoskeletal pain can lead to overlapping risk problems that can cause the body to be misaligned and dysfunctional. Hence why numerous therapies help reduce the effects of musculoskeletal pain and help restore the body naturally. Today’s article looks at how musculoskeletal pain affects the body and how treatments like MET can be used as self-help methods to reduce musculoskeletal pain. We utilize valuable information about our patients to certified medical providers using MET therapy to relieve musculoskeletal pain by incorporating various exercises and stretches. We encourage and refer patients to associated medical providers based on their diagnosis while supporting that education is a remarkable and fantastic way to ask our providers the essential questions at the patient’s acknowledgment. Dr. Alex Jimenez, D.C., comprises this information as an educational service. Disclaimer Musculoskeletal Pain Affecting The Body Are you experiencing muscle stiffness or weakness in your back, neck, or shoulders? Do you feel pain when stretching or hunched over due to discomfort? Musculoskeletal pain is a common issue that can interfere with daily activities. Research studies show that this type of pain can cause symptoms that overlap with neuropathic or visceral pain. This means that problems with one muscle or organ in the body can lead to pain in other areas, causing significant discomfort. Further research has shown that musculoskeletal pain can originate in the muscle tissues and persist for over three months, affecting many individuals’ social and emotional skills, work productivity, and independence. Several environmental factors like obesity, stress, poor sleep, inadequate nutrition, and lack of physical activity can overwork the muscles and joints, leading to trigger points and muscle strain in the musculoskeletal system, resulting in bodily misalignment. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Everyone experiences a muscle cramp at some point. A muscle cramp is an involuntarily contracted muscle that does not relax, similar to a spasm, but a cramp lasts longer and is usually a forcible contraction. During a cramp, the muscles tighten without voluntary input from the brain and over-tighten. They can last anywhere from a few seconds to an hour or longer. They can be prevented through adequate nutrition and hydration, attention to safety when engaged in physical activity or exercise, and attention to posture and ergonomics. Injury Medical Chiropractic and Functional Medicine Clinic can develop personalized treatment plans for individuals experiencing musculoskeletal issues. Muscle Cramp Muscle cramps can occur in any muscle. The cramp may involve a portion of a muscle, the entire muscle, or several muscles that function together. A muscle or a few tissue fibers that involuntarily contracts is in a spasm. If the spasm is forcefully sustained, it turns into a cramp. They can cause a noticeable and/or hardening of the involved muscle/s. They can be experienced as mild twitches or can be excruciatingly painful. Some can involve the simultaneous contraction of muscles that normally move body parts in opposite directions. It is not uncommon for a cramp to flare up multiple times until it finally stops. Causes They can occur during physical activity, exercise, rest, or night, depending on the cause. There are various causes that, include: - Dehydration.
- Electrolyte imbalance.
- General overexertion.
- Physical exertion in hot weather.
- Physical deconditioning.
- Medications and supplements.
Most times, they are not a cause for alarm; however, depending on the individual, their age, type of physical activity, and medical history, cramps could indicate a more serious underlying problem such as a thyroid disorder, liver cirrhosis, atherosclerosis, ALS, or a problem or condition of the spine or spinal nerves. Muscles Involved The muscles involved can indicate the mechanism and cause. - If the cramp is triggered by fatigue, a drop in muscle glycogen, dehydration, or an electrolyte imbalance, it's most frequently to the calf muscles, feet, or back of the thigh/hamstring muscles.
- This is typically due to a combination of fatigue and dehydration.
- If it is triggered by nerve irritation, like a spinal disc injury, cramps tend to present in the forearm, hand, calf, and foot, depending on whether the disc injury is in the neck or lower back.
- If there is a joint sprain in the neck, mid-back, or lower back, the cramp will present where the injury is and around the surrounding muscles.
- A calf cramp happens when lying down because the foot points down, shortening the calf muscles.
- A shortened muscle is more likely to go into spasm, especially if it is exhausted from activities and if the body is dehydrated, which is pretty common.
- For two muscles that work together performing the same movement, called agonists, and the one muscle is weaker, the secondary muscle has to work harder, often going into a spasm or cramp from the added stress.
- For example, if the buttock/gluteal muscles are weak, the hamstrings eventually spasm when exhausted.
Chiropractic First, the cause needs to be identified through medical history and examination. There can be an underlying nerve irritation and interference, restricting the muscle or muscle group, which needs to be dealt with for the therapy to be effective. Chiropractic care, combined with therapeutic stretching and massage therapy, can: - Relieve muscle cramping
- Improve blood circulation
- Increase muscle movement
- Improve musculoskeletal function
- All help to diminish and prevent muscle cramping.
Adjustments will restore proper alignment and restore nerve communication. These treatments help to release toxins, loosen and relax the muscle tissues, and provide relief. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.* Our office has reasonably attempted to provide supportive citations and identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, don't hesitate to get in touch with Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Blyton, Fiona, et al. "Non-drug therapies for lower limb muscle cramps." The Cochrane Database of systematic reviews vol. 1,1 CD008496. 18 Jan. 2012, doi:10.1002/14651858.CD008496.pub2 FIELDS, A. "Leg cramps." California Medicine vol. 92,3 (1960): 204-6. Garrison, Scott R et al. "Magnesium for skeletal muscle cramps." The Cochrane Database of systematic reviews vol. 9,9 CD009402. 21 Sep. 2020, doi:10.1002/14651858.CD009402.pub3 Katzberg, Hans D. “Case Studies in Management of Muscle Cramps.” Neurologic clinics vol. 38,3 (2020): 679-696. doi:10.1016/j.ncl.2020.03.011 Miller, Kevin C et al. "An Evidence-Based Review of the Pathophysiology, Treatment, and Prevention of Exercise-Associated Muscle Cramps." Journal of athletic training vol. 57,1 (2022): 5-15. doi:10.4085/1062-6050-0696.20 Miller, Timothy M, and Robert B Layzer. "Muscle cramps." Muscle & nerve vol. 32,4 (2005): 431-42. doi:10.1002/mus.20341
Introduction We are constantly on the move throughout the day, from walking, running, or standing doing errands, all because of the lower and upper portions of our bodies. The body is a complex, unique machine with upper and lower portions with specific jobs and functions. The body’s upper portion provides mobility and functionality to the neck, shoulders, head, arms, and hands. At the same time, the lower portion of the body offers stability and motor functions to the hips, legs, knees, and feet. When there are issues that affect the body, it can, over time, causes stress in the musculoskeletal system and affect the joints in the lower extremities, thus invoking pain and disability. Today’s article looks at tibial stress fractures, how they affect the lower body, and how treatments like the MET technique can help the lower body. We provide and mention valuable information about our patients to certified medical providers who offer therapy techniques like the MET combined with treatment care for individuals with tibial stress fractures in their lower body extremities. We encourage each patient by referring them to our associated medical providers based on their findings appropriately. We acknowledge that education is a spectacular way when asking our providers the most helpful questions at the patient’s acknowledgment. Dr. Alex Jimenez, D.C., utilizes this information as an educational service. Disclaimer What Are Tibial Stress Fractures? Have you been dealing with heaviness in your legs and feet? What about unwanted pain radiating from your knees to your shin? Or do your feet constantly feel tired? Many of these issues could be due to muscle overload on the lower extremities associated with tibial stress fractures. Research studies reveal that when the lower extremities are subjected to repeated mechanical stress, that can cause microscopic fractions in the tibia. This condition is most common in military recruits, athletes, and runners. In the book “Clinical Applications of Neuromuscular Techniques” by Leon Chaitow, N.D., D.O., and Judith Walker DeLany, L.M.T., stated that two types of stress fractures can occur in the tibia that is the result of tibial stress fractions. They are: - Fatigue stress fracture: Caused by repeated abnormal muscular stress (torque) applied to the normal bone, which has appropriate elastic resistance potential and density.
- Insufficiency stress fracture: Caused by normal muscular forces applied to mineral-deficient or abnormally inelastic bone.
How Do They Affect The Lower Body? Numerous factors can cause stress fractures in the lower body extremities, affecting motor-sensory and mobility function. Some of the factors associated with stress fractures in the tibia include: - A sudden increase in training or activities
- Uneven surfaces
- Inappropriate footwear
- Inappropriate running style
- Misalignment in the lower limbs
Studies have revealed that when these risk factors cause the development of stress fractures in the legs, it can lead to symptoms like pain and swelling in the legs and feet. If it continues without treatment over time can cause the bones to weaken and can be confused with musculoskeletal disorders like osteoporosis or shin splits. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Introduction Many people don’t often realize that stability and balance are two of the most reliable abilities to keep the body from falling, and it is often taken for granted from the earlier stages, where infants and toddlers are learning to stand upright, to adulthood where we are walking, running or performing any physical activities. Our bodies are complex machines comprised of upper and lower portions that provide balance and stability. The lower half of our bodies helps stabilize and balance the upper half weight and allows us to move around. This is known as gait. However, when the body begins to age naturally or chronic issues begin to affect the muscles and cause an imbalance in the lower half, it can lead to many disorders associated with these imbalances. Today’s articles examine what gait is, how gait disturbances are associated with the body, and how the MET technique improves gait. We provide information about our patients to certified medical providers that offer available therapy techniques like MET (muscle energy techniques) for individuals dealing with chronic conditions associated with gait disturbances that could affect a person’s ability to walk. We encourage each patient appropriately by referring them to our associated medical providers based on their diagnosis results. We accept that education is a spectacular way when asking our providers the most crucial questions at the patient’s acknowledgment. Dr. Alex Jimenez, D.C., assesses this information as an educational service. Disclaimer What Is Gait? Have you been dealing with issues when walking for a short or long distance? Do your feet or ankles seem to feel tired or ache when stepping? Or have you been dealing with mobility issues in your hips? Many of these issues are associated with gait and can cause balance disturbances in the body. So what is gait? In the book by Leon Chaitow, N.D, D.O., and Judith Walker DeLany, L.M.T, titled “Clinical Applications of Neuromuscular Techniques,” gait is defined as how you walk and how each lower body section contributes to how you walk. This includes: - Feet
- Ankles
- Knees
- Hips
- Spine
The book also mentions how a person progresses from one location to another using muscular action and gravity to make them walk. Two functional units are in a casual relationship contributing to gait: the passenger and locomotor units. The passenger unit consists of the upper extremities, like the head, neck, arms, trunk, and pelvis, to be the center of gravity when moving forward. At the same time, the locomotor unit comprises the pelvis and lower extremities, like the legs, knees, feet, and ankles, to support the weight of the upper extremities and perform structural stability and mobility to make the body move forward. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Flexibility is the ability of joint/s to move through an unrestricted range of motion. To maintain joint health, the cartilage and structures within the joint need a constant supply of blood, nutrients, and synovial fluid to move through a full range of motion. The range of motion is influenced by the mobility of the soft tissues that surround the joint. These soft tissues include muscles, ligaments, tendons, joint capsules, and skin. Factors affecting the loss of normal joint flexibility include injury, inactivity, or little to no stretching. Although flexibility varies for everybody, minimum ranges are necessary for maintaining total body health. Injury Medical Chiropractic and Functional Medicine Clinic can create a personalized stretching program to restore joint flexibility. Joint Flexibility Body Effects - Not stretching the body can lead to fatigue, weakness, and soft tissue shortening.
- The effect can be particularly noticeable in weight-bearing joints like the hips and knees.
- If the joints become weak, the risk of injury increases.
- Inflexible muscles tire more quickly, causing opposing muscle groups to work harder.
- Muscle fatigue can lead to muscular injuries and the inability to protect the joints from more severe injuries.
- Decreased flexibility can also lead to added stress on structures and tissues in a different body area from the source of the inflexibility.
- An example is tendonitis in the knee can be related to calf tightness.
Stretching Routine Benefits Research has shown that stretching can help improve flexibility and, as a result, the range of motion of the joints. Benefits include: - Improved performance in physical activities.
- Improved ability with daily activities.
- Decreased risk of injuries.
- Increase circulation.
- Improved muscle function.
Testing Flexibility can be measured with functional tests. These tests measure the joint's range within common movement patterns. Using these tests, areas of inflexibility can be identified and addressed. The tests look at the following: - Neuromuscular coordination.
- How the muscles return to a normal resting state.
- Blood circulation and recirculation.
- Typical assessment areas include the lower back, hips, hamstrings, knees, and feet.
Stretching the Body Developing a regular stretching routine to be incorporated into a training program is recommended. A stretching routine should cover all the major muscle groups of the body as well as any specific muscle groups. Implementing a physical therapy stretching program can help individuals stay motivated, as gaining flexibility takes time. It can take several weeks of consistent, regular stretching for improvement. - Stretching with a physical therapist will target the largest areas of inflexibility.
- Stretching sessions can be 20 minutes or more.
- Once these areas have been addressed, the therapist will move on to more specific areas.
- The therapist will train the individual how to stretch at home.
The therapist will provide specific guidelines that should be followed for stretching at home: - Stretching when muscles are cold could lead to a strain or pull.
- Warming up before stretching is recommended as it increases the blood flow and temperature of the muscles, ligaments, and tendons, improving the elasticity and functioning of the tissues.
- Begin each stretch slowly and gently.
- Maintain the stretch position for 30 seconds, and gradually increase to 1-2 minutes.
- Maintain a regular breathing pattern when stretching.
- Stay relaxed, and do not bounce.
- There should be pulling or tightness but not pain.
- Static stretching should gradually go through the full range of motion until the resistance is felt.
- Stretch to the point of tightness and then just beyond.
- Gradually release the stretch.
- Repeat daily.
A stretching therapy program keeps the body loose and effectively increases the mobility of all soft tissues. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.* Our office has reasonably attempted to provide supportive citations and identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please contact Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Behm DG. Does stretching affect performance? In: The Science and Physiology of Flexibility and Stretching. Kindle edition. Routledge; 2019. Berg, K. Stretching fundamentals. In: Prescriptive Stretching. 2nd ed. Kindle edition. Human Kinetics; 2020. Ghasemi, Cobra, et al. "The effect of soft tissue manipulation and rest on knee extensor muscles fatigue: Do torque parameters and induced perception following muscle fatigue have enough reliability?." Journal of family medicine and primary care vol. 9,2 950-956. 28 Feb. 2020, doi:10.4103/jfmpc.jfmpc_838_19 Gordon BT, et al., eds. Flexibility assessments and exercise programming for apparently healthy participants. In: ACSM's Resources for the Exercise Physiologist. 3rd ed. Kindle Edition. Wolters Kluwer; 2022. Hui, Alexander Y et al. "A systems biology approach to synovial joint lubrication in health, injury, and disease." Wiley interdisciplinary reviews. Systems biology and medicine vol. 4,1 (2012): 15-37. doi:10.1002/wsbm.157 Lindstedt, Stan L. "Skeletal muscle tissue in movement and health: positives and negatives." The Journal of experimental biology vol. 219, Pt 2 (2016): 183-8. doi:10.1242/jeb.124297
Introduction The hips in the lower portions of the body allow the legs to move the host from one location to another and provide stability to support the upper body’s weight. The hips will enable the torso to twist and turn without feeling pain. This is due to the various muscles and ligaments surrounding the pelvic bone and hip joint socket that allow the motion to be possible. However, when various injuries or factors start to affect the multiple muscles surrounding the pelvis or there is a chronic condition like osteoarthritis that causes wear and tear on the hip joints can cause underlying symptoms associated with the hips and cause many individuals to have difficulty when moving around. Luckily there are ways to improve hip mobility and the surrounding muscles in the hip and pelvic region of the body. Today’s article looks at the causes of the development of tight hips in the body and how different stretches can release tight hip flexor muscles. We refer our patients to certified providers that incorporate techniques and multiple therapies for many individuals suffering from hip pain and its correlating symptoms that can affect the musculoskeletal system in the hips, legs, and lumbar region of the spine. We encourage and appreciate each patient by referring them to associated medical providers based on their diagnosis when it is appropriate. We understand that education is a fantastic way when asking our providers intricated questions at the patient’s request and understanding. Dr. Jimenez, D.C., only utilizes this information as an educational service. Disclaimer What Causes The Body To Develop Tight Hips? Have you been dealing with hip mobility issues? When you sit, do you feel uncomfortable, and your hip muscles become tight? Or do you have a decreased range of motion when moving your hips? It could correlate with your hips if you have been experiencing muscle pain issues in the lower extremities. The hips help stabilize the upper and lower portions of the body while providing the full leg’s range of motion. When a person begins to sit for long periods or twist their body in a weird position, it can cause the muscles that surround the hips to become shortened. Other issues, like chronic conditions, can play a role in developing tight hip flexors. Studies reveal that various pathologies affecting the hips, lumbar spine, and lower extremities could strongly correlate with restricted hip mobility that can cause harmful effects that can affect the hips. To that point, some of the symptoms associated with tight hip flexors include: - Instability
- Hypermobility
- Limited range of motion
- Reduce muscle strength in the groin
- Muscle cramps
- Sharp, sudden pain in the hips, pelvis, or groin
- Low back pain
- Piriformis syndrome
Other research studies mentioned that hypermobility disorders could affect the hip joints. Hypermobility disorders like EDS (Ehlers-Danlos syndrome) could cause micro or macro-trauma on the hip joint and affect the ligaments surrounding the hip joint. To that point, it can cause the hip flexor muscles to become tense and potentially affect how a person moves, which then causes soft tissue injuries and chronic pain. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Introduction The various muscles and tendons surrounding the foot play an important role as they provide stability to the lower parts of the body and allow the individual to move and flex their feet. These various muscles and tendons help support the ankles and allow leg movement. Many people will be on their feet constantly as the world moves and sometimes have to deal with various issues affecting their ability to walk. As the body naturally ages, many people will begin to shuffle their feet around, which causes strain on the foot muscles and can affect the calves and legs over time. To that point, it can lead to foot pain and other conditions that can affect the individual. Other issues that can affect the feet and its muscle could be incorrect footwear, how they are standing, or how they walk. When this happens, conditions like plantar fasciitis and trigger point pain can affect the feet differently. Today’s article focuses on the superficial intrinsic foot muscles, how trigger points and plantar fasciitis correlate with foot pain, and how to strengthen the foot muscles. We refer patients to certified providers incorporating techniques and therapies in the lower body extremities of trigger points affecting the feet. This helps many people with trigger point pain symptoms associated with plantar fasciitis along the intrinsic foot muscles. We encourage and appreciate each patient by referring them to associated medical providers based on their diagnosis when it is appropriate. We understand that education is a terrific way when asking our providers intricated questions at the patient’s request and understanding. Dr. Alex Jimenez, D.C., only utilizes this information as an educational service. Disclaimer The Superficial Intrinsic Foot Muscles As stated earlier, the foot has various muscles and tendons that allow stability to the ankles and allow movement when a person is walking. The foot has two muscle groups: the extrinsic and intrinsic muscles. Today we will look at the intrinsic foot muscles and how important these muscles are in the foot. Studies reveal that the intrinsic foot muscles are highly important as they are contained to the foot and contribute to supporting the medial longitudinal arch. The intrinsic foot muscles are superficial and help keep the toes straight while providing flexion and extension when in motion. The foot has about 29 muscles, including 10 surrounding the foot and ankle, while the other 19 are intrinsic and provide the roles for gait and posture. The 19 intrinsic muscles have the following: - Abductor Hallucis
- Quadratus Plantae
- Flexor Hallucis Brevis
- Flexor Digitorum Brevis
- Abductor Digiti Minimi
- Flexor Digiti Minimi
- The Interossei Muscles
- The Lumbricals
These muscles allow individuals to walk, run, or jog without pain. However, when the intrinsic muscles become impaired, studies reveal that intrinsic foot muscle function could be linked to various foot conditions that affect a person’s walking ability. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Introduction The feet allow movement to make the host do various actions when it comes to the body. Whether running, walking, or stretching, the feet allow stability with help from the legs and lower limbs of the lower body to support the upper body’s weight and allow mobility and functionality to the hips. The feet have various extensor muscles that start at the head where the tibia and in the front of the shin and spreads out to the front of the foot and allow movement to each of the toes. Injuries like ankle sprains, objects landing on the foot, or muscle cramps can cause the various muscles to become injured and soon develop tiny nodules that can cause referred pain to the lower portion of the legs and cause mobility issues. To that point, trigger point pain can affect how a person functions and cause many to deal with unquestionable foot pain. Today’s article looks at the extensor muscles of the toes, how trigger points can affect the foot and toes, and how chiropractic care can help treat trigger points along the extensor muscles of the toes. We refer patients to certified providers that incorporate various techniques in the lower body extremities, like lower legs, calves, and foot pain therapies correlating to trigger points. This helps aid many people with pain symptoms along the extensor toe muscles, causing pain when doing everyday actions like stepping or walking. We encourage and appreciate each patient by referring them to associated medical providers based on their diagnosis when it is appropriate. We understand that education is a terrific way when asking our providers intricated questions at the patient’s request and understanding. Dr. Alex Jimenez, D.C., only utilizes this information as an educational service. Disclaimer The Extensor Muscles Of The Toes Have you been having issues walking for long periods? Do your feet constantly ache, so you have to take off your shoes to rub them? Or have you been having mobility issues that start at the hips and then travel down to the feet? Many of these issues are associated with pain that can affect the extensor muscles of the toes. The feet have various superficial muscles that allow movement to each toe. Today, we will look at the extensor muscles that enable movement to the toes and help with lower limb functionality. The extensor toe muscles include the extensor digitorum and the extensor hallucis longus. Studies reveal that the extensor muscles are the anterior compartment of the lower limbs that can allow extension and dorsiflex of the foot at the ankle. The extensor hallucis provides movement to the big toe, independently moving it up and down. At the same time, the extensor digitorum forms into four tendons to the other toe joints. These muscles work together to control the foot when descending and allow the heel to land first and then the toes after to prevent foot slaps or hard stepping. To that point, during this gait action, the extensor digitorum helps provide pure dorsiflex of the foot through balance on the tibial muscle. In contrast, the extensor hallucis allows the foot to adapt when the host is walking. Now, what happens when the extensor muscles suffer from injuries that cause mobility issues to the individual? General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Introduction The calves are extremely important to the lower portions of the legs as they allow the individual to move around and help stabilize the entire body. The calves have two muscles: the gastrocnemius and the soleus, which provide plantarflexion and stability at the ankle joint. These two muscles work together to ensure that the upper body’s weight doesn’t lean forward too much to let the individual fall. However, when many people overuse the calf muscles constantly, it can cause the muscle fibers in the lower legs to be overstretched and develop small nodules known as trigger points to cause referred pain to the calves and the ankles that can affect a person’s ability to walk, run, or jump. Today’s article looks at the soleus muscle, how trigger points affect the muscle, and different methods to reduce pain while managing trigger points along the calves. We refer patients to certified providers that incorporate various techniques in the lower body extremities, like lower leg and calve pain therapies correlating to trigger points, to aid many people dealing with pain symptoms along the soleus muscles, causing muscle cramps and issues along the ankles. We encourage and appreciate each patient by referring them to associated medical providers based on their diagnosis when it is appropriate. We understand that education is an excellent way when asking our providers intricated questions at the patient’s request and understanding. Dr. Alex Jimenez, D.C., only utilizes this information as an educational service. Disclaimer What Is The Soleus Muscle? Do you feel a cramping sensation in your calves? Do your feet hurt when you are walking, jumping, or running? Or are you experiencing tightness in your calve muscles? When a person is experiencing calf pain in their legs, it could be trigger points causing overlapping issues in the soleus muscles. As stated earlier, the calves have two muscles: the gastrocnemius and the soleus. The gastrocnemius makes up the round shape of the calves and is a complex, superficial muscle. At the same time, the soleus is a large, flat muscle deep within the gastrocnemius and forms the calcaneal tendon (Achilles tendon), which can be mistaken as a nerve for the ankle. Studies reveal that the soleus muscle works together with the gastrocnemius, and these muscles constitute a plantar flexor. The soleus is part of a group of muscles known as antigravity muscles. It acts like a skeletal muscle and helps maintain good posture in the body to prevent the sheer body weight from falling forwards at the ankle when standing. How Do Trigger Points Affect The Soleus Muscle? The calves are essential for the movement and mobility functions of the body. When the calve muscles have been overused to repetitive movements or have been dealing with trauma, it can cause the muscle fibers to tear and develop trigger points along the calves causing referred pain to travel down the ankles. Trigger points along the soleus muscle are tricky to diagnose since they cause referred pain to the surrounding muscles. “Myofascial Pain and Dysfunction,” written by Dr. Janet G. Travell, M.D., mention that, unlike the latent trigger points that can affect the gastrocnemius, active trigger points can affect the soleus muscle and cause tenderness referred to the heel. When muscle tenderness affects the heels, it can cause trigger points to mimic chronic conditions like plantar fasciitis. Additional studies reveal that musculoskeletal impairments like trigger points in the soleus muscle could potentially lead to biomechanical changes in the ankle. When trigger points cause hypersensitivity spots in the skeletal muscle taut band, it can restrict the soleus muscle to allow ankle dorsiflexion. Individuals with active soleus trigger points are prone to develop low back pain due to ankle dorsiflexion restriction, leading to them leaning over and lifting objects improperly. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Introduction The hips and thighs have a working relationship as their jobs are to maintain stability for the legs and pelvis while supporting the upper body’s weight. These two body groups have various muscles, tendons, and nerves that have specific jobs that allow mobility to the lower body. Many athletes in multiple sports events use their thighs to exert a huge amount of power to be the best. This is due to the adductor muscles in the thighs that allow the athlete to win the event. These adductor muscles are voluminous in size and can become overstretched if the muscles have been worked out too much or injuries have caused dysfunction in the surrounding muscles, causing mobility issues. To that point, the adductor muscles will develop myofascial trigger points and cause hip and thigh pain. Today’s article looks at the two adductor muscles (Longus and Magnus), how myofascial trigger points affect the adductor muscles, and available treatments to manage hip adductor trigger points. We refer patients to certified providers who incorporate multiple methods in the lower body extremities, like thigh and hip pain treatments correlating to myofascial trigger point pain, to aid individuals dealing with pain symptoms along the adductor muscles. We encourage and appreciate patients by referring them to associated medical providers based on their diagnosis, especially when appropriate. We understand that education is an excellent solution to asking our providers complex questions at the patient’s request. Dr. Jimenez, D.C., utilizes this information as an educational service only. Disclaimer Adductor Longus & Adductor Magnus Have you been dealing with groin pain located near your thighs? Do you feel muscle tenderness or stiffness when stretching your inner thighs? Or have you been feeling unstable in your hips or thighs when walking? Many individuals, especially athletes and older adults, could be experiencing myofascial trigger points associated with groin pain along their adductor muscles. The thighs contain several muscles and functions that allow many people to bend and extend their knees and hips. The adductor muscles allow the legs to move inward toward one another. The adductor muscles have five muscles: magnus, brevi, longus, pectineus, and gracilis. These muscles enable functionality to the thighs and hips, and we will look at two adductor muscles in the inner thighs. The long adductor muscle is a large, fan-shaped muscle that starts from the superior aspect of the pubis bone and travels down to connect at the thigh bone. Studies reveal that the adductor longus is a long and thin muscle with many actions for the thighs, including external/lateral rotation and thigh flexion. Now the adductor Magnus is a large triangular-shaped muscle of the inner thighs that are important for thigh and hip function and stabilizing the pelvis. Studies reveal that even though the adductor Magnus is a large muscle in the inner thighs, its primary function is to allow the thigh to move in a larger range of motion without any pain inflicted on the thigh muscles. However, the adductor muscle can succumb to various issues affecting the thighs and groin regions of the body that can be overstretched and strain the body. Myofascial Trigger Points Affecting The Adductor Muscles Groin pain is a multi-factorial pain issue that affects the lower limbs, and its often due to muscle strain in the inner thigh muscles. This pain increases during vigorous activities and when there is a sudden twist in the hips. When the adductor muscles suddenly change in motion when the body is active, they can be overstretched and correlate to myofascial trigger points that can affect the inner thigh and groin regions. According to “Myofascial Pain and Dysfunction,” by Dr. Travell, M.D., patients with active myofascial trigger points in the two adductor muscles (Longus and Magnus) would become frequently aware of the pain in their groin and medial thigh. When the adductor muscles have myofascial trigger points in the inner thigh, diagnosing is difficult since the individual thinks they are suffering from groin pain when the pain is in their inner thighs. To that point, studies reveal that many individuals participating in various sports would suffer from groin pain due to myofascial trigger points affecting the adductor muscles. Luckily, there are multiple treatments to reduce the pain in the adductor muscles. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Introduction When many individuals begin to work out or start training for an event, they incorporate various muscles to give optimal output and strength when doing a set of exercises. Many athletes or individuals trying to train for an event or to better themselves have to do a pre-workout routine involving various stretches to warm up the muscles before the actual workout and do stretches post-workout again. This ensures that the muscles are ready to give it their all when a person is working out. The body has various parts with different functions and jobs that help the body’s motor function. The upper body has the shoulders, arms, hands, elbows, neck, head, and chest to allow movements and stability. At the same time, the lower body has the hips, low back, thighs, legs, knees, pelvis, and feet to support the upper body’s weight and stabilize the lower extremities from collapsing. When various factors affect the body, it can lead to dysfunction and causes referred pain to different body locations that can mask chronic conditions. Today’s article looks at one of the lower body muscles located at the inner thighs, known as the pectineus muscle, how trigger point pain affects the inner thighs, and various stretches to strengthen the hip adductors. We refer patients to certified providers who incorporate multiple methods in the lower body extremities, like thigh and hip pain treatments correlating to trigger point pain, to aid individuals dealing with pain symptoms along the pectineus muscle. We encourage and appreciate patients by referring them to associated medical providers based on their diagnosis, especially when appropriate. We understand that education is an excellent solution to asking our providers complex questions at the patient’s request. Dr. Jimenez, D.C., utilizes this information as an educational service only. Disclaimer What Is The Pectineus Muscle? Have you been experiencing pain in your inner thighs? Do you find it difficult to play various sports? Do you feel tenderness or soreness in your thighs or near your groin? Most of these symptoms are associated with trigger point pain along the pectineus muscles that affect the thighs. The pectineus is part of the anterior thigh muscles that extend the leg to the knee joint. The pectineus works with another muscle known as the sartorius and a muscle group known as the quadriceps femoris. The pectineus muscle is responsible for flexion, adduction, and medial rotation since it is a hip adductor for the thighs. This muscle is important for various sports activities like running, skating, soccer, or basketball and can become overused due to overstretching the legs too far, thus developing trigger points in the pectineus muscle. Trigger Point Pain Affecting The Inner Thighs When athletes overuse their legs and overstretch the pectineus muscle, it can cause issues with the thighs, hips, and legs’ mobility causing referred pain to the lower body. This is known as trigger point pain and can be challenging when diagnosing where the pain is located. Studies reveal that trigger point pain affecting the inner thighs, especially the pectineus muscle, can mimic groin and hip pain, causing various symptoms in the lower extremities. The multiple symptoms can include: - Weak adductor muscles
- Muscle fatigue
- Decreased range of motion
- Leg-length discrepancy
Various reasons can lead to the development of trigger point pain associated with the inner thighs along the pectineus; according to “Myofascial Pain and Dysfunction,” written by Dr. Janet G. Travell, M.D., stated that when patients are dealing with pectineus trigger points would complain about the referred pain surrounding the muscle but not the muscle itself. The book also mentioned that nerve entrapment could also be an issue since trigger points like to mimic other chronic conditions. Trigger points along the pectineus muscle can also develop associated with hip joint diseases like advanced osteoarthritis. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Introduction The thighs in the lower half of the body work together with the hips to stabilize the legs when the body is in motion. The thighs and the hips also support the weight of the upper half of the body and are surrounded by muscles, ligaments, and nerve roots to supply blood and sensory-motor function to the legs. One of the thigh muscles that work with the hips is the tensor fasciae latae (TFL) muscle. When the thigh muscles are being overused or suffer from injuries, tiny nodules known as trigger points (myofascial pain syndrome) can affect a person’s ability to function worldwide. Today’s article examines what the tensor fasciae latae muscles do, how myofascial pain syndrome affects the thighs, and various stretches/techniques for the thighs. We refer patients to certified providers who incorporate multiple methods in the lower body extremities, like thigh pain treatments correlating to trigger points, to aid individuals dealing with pain symptoms along the tensor fasciae latae muscle. We encourage and appreciate patients by referring them to associated medical providers based on their diagnosis, especially when it is appropriate. We understand that education is an excellent solution to asking our providers complex questions at the patient’s request. Dr. Jimenez, D.C., utilizes this information as an educational service only. Disclaimer What Does The Tensor Fasciae Latae Muscle Do? Do you have difficulty walking for a long period? So you feel that your hips feel unstable when you move? Or do you feel radiating pain down from your thighs to your knees? Thigh pain associated with these symptoms can affect a person’s ability to move around from one location to another due to trigger points affecting the tensor fasciae latae muscle. The tensor fasciae latae (TFL) muscles are located at the proximal anterolateral thigh and originate from the anterior superior iliac spine. The TFL muscle is between the superficial and deep muscle fibers of the iliotibial (IT) band, as its attachment assists with knee flexion and lateral rotation. The TFL muscles also work together with the gluteus muscles in various hip movements. Studies reveal that the primary function of the TFL muscles is providing balance to the body’s weight and the non-weight-bearing leg to walk. The TFL muscles allow the individual to walk, run, and assist with movement and stabilization to the hips and knees without pain inflicted on the joints and muscles. Myofascial Pain Syndrome Affecting The Thighs Since the TFL muscles allow the person to walk and run, this muscle can become overused and strained through repetitive motions causing many issues to the hips, knees, and thighs. When these issues affect the TFL muscles, they can develop nodules along the muscle fibers known as trigger points or myofascial pain syndrome. Myofascial pain syndrome is a musculoskeletal disorder that can invoke referred pain in one location of the body while affecting the surrounding muscles in a different body location. Myofascial pain syndrome associated with the TFL muscles can cause issues to the hips, thighs, and knees while affecting a person’s ability to walk. Studies reveal that the prevalence of myofascial pain syndrome on the TFL muscles correlates to pain and disability in the thighs. When myofascial pain syndrome affects the TFL muscles, it can mimic chronic knee osteoarthritis. Even though myofascial pain syndrome is challenging to diagnose, it is treatable through various stretches and techniques. In Dr. Janet G. Travell, M.D.’s book, “Myofascial Pain and Dysfunction,” it mentioned that when patients have active trigger points in their TFL muscles, they become aware of the referred pain affecting their hip joints and are unable to lie comfortably on their sides due to the body-weight pressure pressing on the affected TFL muscle. The book also points out that when pain is referred to from trigger points associated with the TFL muscles, it can be mistaken for pain in the glutes. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Introduction The chest in the body has many functions: it helps provide stability on the shoulders, helps protect the heart and lungs, and bears most of the weight of the rest of the upper body. The chest is home to the pectoralis (major and minor) and the serratus anterior muscles, providing mobility and compression to the chest. As the chest muscles protect the heart and lungs, the other muscles, known as the accessory muscles, aid the heart and lungs regarding respiratory and ventilation. In contrast, the primary chest muscles can not provide that function. The sternalis muscle is one accessory muscle that assists the heart and the lungs. Today’s article examines the sternalis muscle in the chest, how myofascial pain syndrome is associated with the sternalis muscle, and various techniques for managing myofascial pain syndrome on the sternalis muscle. We refer patients to certified providers specializing in chest pain therapies to aid many people suffering from myofascial pain syndrome associated with the sternalis muscle along the chest. We brief patients by referring them to our associated medical providers based on their examination when appropriate. We indicate that education is a great solution to asking our providers profound and complex questions at the patient’s request. Dr. Alex Jimenez, D.C., notes this information as an educational service only. Disclaimer The Sternalis Muscle In The Chest Have you been experiencing respiratory issues that are affecting your chest? What about feeling muscle tightness in the middle of your chest? Or are you experiencing radiating pain traveling down your elbow? These symptoms are often associated with pain caused by trigger points along the chest affecting the sternalis muscle. Studies reveal that the sternalis muscle is an anatomical variant along the anterior thoracic region of the body. The sternalis muscle is located right in the middle of the chest and is toward the end of the pectoralis muscles. “Myofascial Pain and Dysfunction,” written by Dr. Janet G. Travell, M.D., explained that the sternalis muscle often occurs bilaterally or unilaterally in the body and may attach itself either in the pectoralis muscle or the sternocleidomastoid. The sternalis muscle could even become a continuation of these muscles as well. One of the unique functions of the sternalis muscle for the body is that it is an accessory muscle. An accessory muscle refers to various muscles that assist the breathing muscles. Since the sternalis muscle assists the other muscles as an accessory muscle, this muscle help opens the airways to allow more oxygen to the lungs. This muscle is extremely useful when it comes to exercising the body. However, this muscle is superficial and can succumb to various issues that affect the chest and internal organs. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
|
Introduction The musculoskeletal system allows the various muscle groups to surround the bones and joints through ligaments and muscle tissues that help with mobility and stabilizes the skeletal structure from pain. As the body ages naturally, the muscles, bones, and joints get affected as numerous factors begin to cause the body to be dysfunctional. Many of these factors could take a toll on the body and cause bone mass density loss, leading to osteoporosis. A person experiencing osteoporosis can generate overlapping risk profiles affecting the body’s muscles and joints, leading to painful symptoms. Today’s article looks at osteoporosis, how it affects the muscles and joints, and how numerous treatments can help reduce osteoporosis symptoms. We utilize information about our patients to certified medical providers using MET therapy to mitigate the effects of osteoporosis on the musculoskeletal system. We encourage patients by referring them to associated medical providers based on their diagnosis while supporting that education is a remarkable way to ask our providers the most interesting and essential questions at the patient’s acknowledgment. Dr. Alex Jimenez, D.C., comprises this information as an educational service. Disclaimer What Is Osteoporosis? If you’ve been experiencing severe back or hip pain or struggling to breathe, you may be experiencing osteoporosis. This condition causes bones to become porous, making them brittle and weak, and it affects around 200 million people worldwide, with women being more commonly affected than men, as studies revealed. Many risk factors can cause bones to deteriorate quickly and become weaker, leading to an increased risk of fragility, fracture, and muscle and joint pain. Additional studies have revealed that some risk factors that can lead to osteoporosis development include: - Race
- Ethnicity
- Age
- Sex
- Metabolic syndrome
Osteoporosis can often go undetected for a long time, with individuals only noticing symptoms such as a forward-curved upper back or a broken bone. Osteoporosis Affecting The Muscles & Joints Osteoporosis can affect the body’s bones, muscles, and joints, especially major skeletal portions like the spine, hips, wrists, and shoulders. Studies have shown that individuals with or without trauma can experience symptoms like pain due to osteoporosis caused by hormone deficiency. “Clinical Applications of Neuromuscular Techniques” by Dr. Leon Chaitow, N.D., D.O., and Dr. Judith Walker DeLany, L.M.T., explain that bone density can decrease when bone resorption happens faster than bone formation. This decrease in bone density could lead to joint fractures and cause musculoskeletal disorders that affect a person’s stability and mobility, leading to complaints in the upper and lower body extremities. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Introduction The muscles surrounding the hips in the lower extremities provide stability to the lumbar spine and pelvis while allowing mobility, flexibility, and rotation to the groin, legs, and thighs. The muscles surrounding the groin consist of three large muscle groups: the abdominals, iliopsoas, and adductors, which have a casual relationship with the various ligaments and soft tissues that can be succumbed to injuries or other symptoms that can lead to pain and misalignment to the body. This happens to many individuals who participate in sports or frequently exercise, which can cause strain near the groin and the surrounding muscles. Today’s article focuses on the causes of a groin strain, how it affects the hips and pelvis, and how available treatments can help reduce groin strain. We mention and provide valuable information about our patients to certified medical providers who use techniques like the MET and therapy for individuals with a groin strain and causing mobility issues when functioning. We give encouragement to patients by referring them to associated medical providers based on their diagnostic findings. We support that education is a marvelous way to ask our providers the most interesting questions at the patient’s acknowledgment. Dr. Alex Jimenez, D.C., incorporates this information as an educational service. Disclaimer The Causes Of Groin Strain Have you experienced any mobility issues when walking? Do you feel pain near your hips or groin? Or do you feel muscle weakness in your thighs when exercising? Many of these issues are associated with a muscle strain near the groin affecting your lower body. The muscles surrounding the groin allow the legs and thighs to move around in flexion, rotation, and extension without feeling pain. However, when a person starts to feel pain radiating around their groin, it can become an issue if not taken care of. Studies reveal that some of the causes, like adductor strain or injuries from physical activities, can cause the muscle fibers in the three muscle groups of the groin to be in pain. In “Clinical Applications of Neuromuscular Techniques,” authors Leon Chaitow and Judith Walker DeLany, stated that chronic joint and soft tissue conditions predate presenting acute symptoms to the groin muscle regions. To that point, if a person has predisposed injuries in the groin muscles, it can affect how a person walks and functions when in motion, potentially leading to issues affecting the hips and pelvis. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Resistance band exercises can be very useful for injury rehabilitation. As a part of a chiropractic neuromusculoskeletal treatment plan, personalized rehabilitation exercises using resistance bands can be prescribed to strengthen targeted areas of the body that require retraining due to an injury or condition. Resistance band training can effectively rehabilitate neck, shoulder, back, leg, knee, and ankle conditions and offer several advantages, from improving strength and posture to increasing mobility and improving joint health. Resistance Bands Resistance bands are rehabilitation and exercise equipment that provide consistent resistance throughout a specific exercise. They are rubberized bands or elastic cables that can be color-coded (different brands may vary in color progressions) to signify the amount of resistance they provide. These bands are great for all types of injuries to the joints or muscles and have been found to be effective in the following types: - Weakened neck muscles from injury.
- Shoulder dislocation
- Tennis elbow
- Hip bursitis
- Knee injuries
- IT band syndrome
- Ankle sprains
- Improve flexibility for arthritis.
The body does need time to heal before engaging in exercise, especially after major muscle, ligament, or tendon tears. A chiropractor or physical therapist will inform the patient when they can begin. However, some areas can be worked out three days after an injury. Benefits Resistance bands can isolate strength training and stretching to specific muscles affected by surgery or a non-surgical injury/condition in chiropractic and physical therapy. They can help in the following: - Increased circulation.
- Increased range of motion and flexibility.
- Increased muscular strength.
- Improved posture.
- Increased joint stability.
- Improved balance.
Added benefits: - They are small, lightweight, and portable making them perfect for those that travel frequently.
- They are simple to use.
- They are cost-effective.
- They provide a whole-body workout.
- They come in different resistance levels to progress gradually.
- Safe for every fitness level.
Exercises Exercises with bands can be used in standing, sitting, or lying down positions. Some may consist of movements with resistance coming from body weight. Other activities may require additional resistance. Lunges are an example of a simple exercise to help rehabilitate certain back conditions. Injury Stages Strength and resistance training is essential for healing from neuromusculoskeletal injuries and overall health. Early/Acute Stage - This stage entails light, gentle exercising that will allow damaged tissues to begin healing with simple movements to get circulation moving through the areas.
Second Stage - Physical therapy exercises involving resistance bands.
- This gradually increases the weight on the injured bone, ligament, or muscle so the tissue can develop the ability to withstand strains from daily activities.
Late/Functional Stage - This is the final step, in which the tissues are stressed through functional exercises to be fit enough to return to work, sports, and activities.
General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.* Our office has reasonably attempted to provide supportive citations and identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, don't hesitate to get in touch with Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Lee, Jae-Kwang, and Jae-Hong Lee. “Effect of the lumbar stabilization exercise on the height difference between shoulders and range of motion in older adults.” Journal of physical therapy science vol. 35,1 (2023): 46-50. doi:10.1589/jpts.35.46 Mikesky, A E et al. “Efficacy of a home-based training program for older adults using elastic tubing.” European journal of applied physiology and occupational physiology vol. 69,4 (1994): 316-20. doi:10.1007/BF00392037 Seguin, Rachel C et al. “The Efficacy of Upper-Extremity Elastic Resistance Training on Shoulder Strength and Performance: A Systematic Review.” Sports (Basel, Switzerland) vol. 10,2 24. 14 Feb. 2022, doi:10.3390/sports10020024 Seo, Myong-Won et al. “Effects of 16 Weeks of Resistance Training on Muscle Quality and Muscle Growth Factors in Older Adult Women with Sarcopenia: A Randomized Controlled Trial.” International journal of environmental research and public health vol. 18,13 6762. 23 Jun. 2021, doi:10.3390/ijerph18136762 Yamamoto, Yutaro, et al. “Effects of resistance training using elastic bands on muscle strength with or without a leucine supplement for 48 weeks in elderly patients with type 2 diabetes.” Endocrine journal vol. 68,3 (2021): 291-298. doi:10.1507/endocrj.EJ20-0550
Spinal Stenosis Walking Issues: Stenosis means a narrowing. Spinal stenosis can happen in any spine region, but the neck and lower back are the most common locations. The spinal canal becomes narrower and can cause the nerves to become compressed, pinched, and irritated and can extend from the lumbar spine through the hips, buttocks, legs, and feet. Individuals with lumbar spinal stenosis may have difficulty walking caused by sensations of discomfort like numbness, electrical shocks, and pain, requiring the need to lean forward to relieve pressure and symptoms. Additionally, symptoms are likely to worsen the longer the walk. Chiropractic treatment can treat spinal stenosis because it corrects and re-aligns the spine, thus reducing pressure on the spinal cord, joints, and nerve roots. Spinal Stenosis Walking Issues The spine is made up of interlocking vertebrae. The regions are cervical, thoracic, lumbar, and sacral bones with a foramen opening. These openings form the protective tunnel/spinal canal surrounding the spinal cord. The spinal cord is a group of nerves that run through the tunnel. The narrowing suffocates the nerves supplying the lower extremities that can influence walking activity. Symptoms There may be no symptoms with early lumbar spinal stenosis. Most individuals develop symptoms gradually and may begin to notice them while walking or standing. These can include: - Lower back pressure sensations when standing upright or walking.
- Leg numbness, tingling, weakness, burning, and/or cramping.
- Muscle weakness.
- Persistent pain in the back, hips, buttocks, or legs while walking.
- Difficulty lifting the top part of the foot - known as drop foot.
- Loss of sensation in the feet.
- A weak foot that drops/slaps down when walking.
- Loss of sexual ability.
- In more serious cases, severe numbness, bladder problems, and inability to stand.
Individuals begin to lean forward when symptoms start, bringing relief by reducing the pressure on the nerves. However, constantly leaning forward leads to other posture and health problems. Diagnosis A doctor or chiropractor will ask questions about symptoms and medical history and perform a complete physical examination to diagnose lumbar spinal stenosis. During the physical examination, a healthcare provider will look for signs, such as loss of sensation, weakness, and abnormal reflexes. Tests: - X-rays of the lumbar spine may show bone growths called spurs that push on spinal nerves and/or narrowing of the spinal canal.
- Imaging tests - A CT or MRI scan can provide a detailed look at the spinal canal and nerve structures.
- Other studies include - bone scans, myelogram, which is a CT scan that uses a color dye, and EMG, which is an electrical test of muscle activity.
Chiropractic Treatment Chiropractic care combined with physical therapy is a tried-and-true treatment for spinal stenosis. A chiropractic treatment plan can include targeted and passive exercise programs. Targeted exercises involve strengthening the core and back muscles. Passive treatments include hot and cold therapy, massage, decompression, and electrical stimulation. The objective of chiropractic therapy is to: - Strengthen muscles in the core and legs
- Correct posture and body mechanics.
- Improve mobility.
- Maintain ability to perform day-to-day activities.
- Recommend stretches.
- Educate on how to keep the spine and back muscles safe.
- Train on using devices like a back brace, cane, or walker properly.
- Advise about shoe inserts and splints.
- Suggest work and home environment modifications, such as ergonomics and cushions.
General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.* Our office has reasonably attempted to provide supportive citations and identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, don't hesitate to contact Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Conway, Justin, et al. “Walking assessment in people with lumbar spinal stenosis: capacity, performance, and self-report measures.” The spine journal: official North American Spine Society journal vol. 11,9 (2011): 816-23. doi:10.1016/j.spinee.2010.10.019 Lurie, Jon, and Christy Tomkins-Lane. “Management of lumbar spinal stenosis.” BMJ (Clinical research ed.) vol. 352 h6234. 4 Jan. 2016, doi:10.1136/bmj.h6234 Macedo, Luciana Gazzi, et al. “Physical therapy interventions for degenerative lumbar spinal stenosis: a systematic review.” Physical therapy vol. 93,12 (2013): 1646-60. doi:10.2522/ptj.20120379 Tomkins-Lane, Christy C et al. “Predictors of walking performance and walking capacity in people with lumbar spinal stenosis, low back pain, and asymptomatic controls.” Archives of physical medicine and rehabilitation vol. 93,4 (2012): 647-53. doi:10.1016/j.apmr.2011.09.023
Having and maintaining flexibility in the joints depends on the connective tissues surrounding the muscles. Proper lubrication in the connective tissues enables the fibers to slide over one another easily. Naturally occurring proteins collagen and elastin are key components of connective tissue that provide strength and elasticity. The more elastic the connective tissue, the more flexibility around the joint. If it is becoming difficult to stretch out or there is chronic stiffness and tightness, there are foods that help maintain flexibility and enhance overall health. Foods That Help Maintain Flexibility Joint flexibility means functioning connective tissues that join the skeleton and muscles and the ability of different body parts to extend and complete motions. Connecting tissues assists with movement and stabilization. These issues include: Ligaments - Ligaments can be band-shaped or string-shaped collagen fibers that connect bones.
Tendons - Tendons are similar to ligaments and are band or string shaped but connect muscles to the bones.
Fascia - Fascia is a densely woven mesh that wraps around the blood vessels, bones, muscles, organs, and nerves.
Flexibility keeps the muscles active and mobile as they are necessary for daily physical activities. When these tissues become stiff from inactivity or an unhealthy diet, it limits the body’s range of movement and increases the risk of injury. Stretching improves flexibility, and adding foods to a nutrition plan will help maintain limberness. Nutrition A nutrition plan full of vitamins, minerals, and antioxidants will nourish connecting tissues and cells and increase collagen production. Foods rich in essential fatty acids/EFAs, vitamin C, sulfur, and water will promote healthy connective tissue for enhanced flexibility. Fatty Acids - Essential fatty acids include omega-3 and omega-6, primarily found in fish, flax seeds, and liquid oils.
- These fatty acids are essential because they cannot be made in the body.
- Foods like fatty fish, flax seeds, walnuts, or supplements, can help achieve the proper ratio.
- For individuals not too keen on fish, consider omega-3 supplements.
Collagen - Collagen is the main protein from connective tissue, and vitamin C is essential for collagen production.
- Vitamin C-rich foods - oranges, bell peppers, broccoli, strawberries, tomatoes, leafy green vegetables, raspberries, pineapple, cruciferous vegetables, parsley, and watermelon.
- Make various smoothie recipes for breakfast or an afternoon snack.
- For increased protein synthesis, add branched-chain amino acids.
Sulfur - Sulfur helps maintain the flexible bonds in connective tissues.
- Animal proteins that provide sulfur include fish, poultry, beef, and eggs.
- Vegetable sources include Brussels sprouts, cabbage, broccoli, cauliflower, onions, and garlic.
Hydration Water is not considered food as it contains no calories, but it is vital as it makes up 76 percent of the muscles. A high percentage of water content is the key to muscle elasticity. When the body is dehydrated, it holds onto water, causing fluid retention and stiffness. The more the muscles stay dehydrated, the more they have trouble recovering from physical activities, fatigue levels increase, the range of motion decreases, and the risk of injury increases. Don’t wait until you are thirsty. Stay hydrated throughout the day to keep the joints lubricated and energy levels high. Fruits high in water include: - Strawberries
- Watermelon
- Cantaloupe
- Peaches
- Grapefruit
- Pineapple
- Apples
- Pears
Vegetables high in water include: - Cucumber
- Lettuce
- Zucchini
- Celery
- Eggplant
Limit Salt and Sugar Intake - Processed foods tend to have a high salt content.
- Too much salt causes the joints to swell as the body retains fluid.
- Keeping sugar intake low is important in enhancing flexibility.
- This is because sugar breaks down the collagen in the skin and connective tissues.
- This means avoiding processed foods, ready meals, and junk food.
Flexibility can be improved by eliminating foods that destroy collagen, focusing on foods that reduce insulin spikes, and maintaining hydration in the connective tissues. A nutritionist can develop a personalized nutrition plan for optimal neuromusculoskeletal health. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.* Our office has reasonably attempted to provide supportive citations and identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, don't hesitate to get in touch with Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Beba, Mohammad et al. “The effect of curcumin supplementation on delayed-onset muscle soreness, inflammation, muscle strength, and joint flexibility: A systematic review and dose-response meta-analysis of randomized controlled trials.” Phytotherapy research: PTR vol. 36,7 (2022): 2767-2778. doi:10.1002/ptr.7477 Kviatkovsky, Shiloah A et al. “Collagen peptide supplementation for pain and function: is it effective?.” Current opinion in clinical nutrition and metabolic care vol. 25,6 (2022): 401-406. doi:10.1097/MCO.0000000000000870 MacKay, Douglas, and Alan L Miller. “Nutritional support for wound healing.” Alternative medicine review: a journal of clinical therapeutic vol. 8,4 (2003): 359-77. Shaw, Gregory, et al. “Vitamin C-enriched gelatin supplementation before intermittent activity augments collagen synthesis.” The American journal of clinical nutrition vol. 105,1 (2017): 136-143. doi:10.3945/ajcn.116.138594 Zdzieblik, Denise, et al. “Improvement of activity-related knee joint discomfort following supplementation of specific collagen peptides.” Applied physiology, nutrition, and metabolism = Physiologie applique, nutrition et metabolism vol. 42,6 (2017): 588-595. doi:10.1139/apnm-2016-0390
Introduction Everyone worldwide knows that feet are important. The feet allow many individuals to run, walk, or jog for long periods without feeling pain for a moderate amount of time. To that point, the various muscles and tendons surrounding the foot provide full body flexion, extension, and stability. Even though it is very easy to get in the recommended amount of steps into being healthy, around 75% of individuals will have foot pain that can impact their ability to walk. One of the most common foot pains is plantar fasciitis, which can become a painful foot condition if it is not treated as soon as possible. Today’s article looks at plantar fasciitis, its symptoms, how trigger points correlate, and treatments for it. We refer patients to certified providers incorporating techniques and therapies for individuals dealing with plantar fasciitis. By locating where the trigger points are coming from, many pain specialists can develop a treatment plan to reduce the effects that plantar fasciitis is causing on the feet. We encourage and appreciate each patient by referring them to associated medical providers based on their diagnosis when it is appropriate. We understand that education is a terrific way when asking our providers intricated questions at the patient’s request and understanding. Dr. Jimenez, D.C., only utilizes this information as an educational service. Disclaimer What Is Plantar Fasciitis? Have you been dealing with constant heel pain? Do you feel pain shooting up your leg when you step or walk? Or do you feel a stabbing ache in your heel? Many of these pain issue people are dealing with correlate with plantar fasciitis. Studies reveal that plantar fasciitis results from degenerative irritation on the plantar fascia and its ligaments. This causes the muscle ligaments to become inflamed, swollen, and weak, which then causes the bottom of the foot or heel to hurt when a person is walking or standing. To that point, when there is a repetitive strain on the feet, it causes microtears in the plantar fascia. The plantar fascia in the foot plays an important role as it comprises three segments that support the medial arch and shock absorption when stepping down. As one of the most common causes of heel pain, the residual pain from plantar fasciitis tends to be a sharp, stabbing sensation. Plantar fasciitis is more prominent in middle-aged people. Still, anyone at any age can develop plantar fasciitis, especially if they have labor jobs requiring them to be constantly on their feet. Symptoms Of Plantar Fasciitis Since around 2 million Americans could potentially develop plantar fasciitis, it is important to know that when a person has been on their feet constantly, there will be inflammation along the tissues in the feet. Many individuals with a busy lifestyle that requires them to be on their feet frequently would often ignore the pain or discomfort. Some of the symptoms that plantar fasciitis causes include the following: - Pain on the bottom of the heel
- Pain in the arch
- Pain that is usually worse when waking up
- Pain that increases over months
- Swelling on the bottom of the heel
However, when the pain becomes overbearing, many people would often think they have sore feet or low back pain from being overly tired from work, under constant stress, or over-exerting their bodies. When this happens, many would think the pain would go away in a few days after resting for a short period. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Introduction Regarding different destinations, our feet allow the legs and the lower body to move forward and stabilize the upper extremities from putting so much weight on the body itself. The lower portion of the body contains the hips, pelvis, legs, and feet. Within each section of the lower body, various muscles surround the joints and skeletal features of the lower half. For the hips, multiple muscles and tendons help support hip mobility and pelvic function. The legs work with the thigh as numerous muscles and tendons help the legs have more power to move. The lower portion of the legs works with the knee to allow extension and flexion to move as well. And finally, the ankles and feet work with various muscles to enable movement to the toes. The different muscles in the toes help stabilize the foot from causing issues to the ankles. However, when multiple injuries or factors begin to affect the muscles in the toes, it can lead to myofascial pain syndrome or trigger points to affect not only the toes but the entire portion of the legs and travel up to the hips. Today’s article looks at the flexor muscles of the toes, how calf pain is associated with trigger points affecting the toes, and how different treatments and stretches can alleviate trigger points along the toe flexor muscles. We refer patients to certified providers that incorporate various techniques and therapies in the lower body extremities pertaining to trigger points affecting the legs, calves, and feet. This helps many people with pain symptoms along the flexor toe muscles, causing pain when doing everyday actions like stepping or walking. We encourage and appreciate each patient by referring them to associated medical providers based on their diagnosis when it is appropriate. We understand that education is a terrific way when asking our providers intricated questions at the patient’s request and understanding. Dr. Alex Jimenez, D.C., only utilizes this information as an educational service. Disclaimer The Flexor Muscles Of The Toes Have you been dealing with stability issues that are affecting the way you are standing? How about coping with unquestionable calf or foot pain? Do you feel aches in your big toe? Many of these issues affecting the feet are correlated with the flexor muscles in the toes. The flexor muscles are the flexor digitorum longus and the flexor hallucis longus. These muscles are located in the calf region of the lower leg and travel downwards to the ankle, forming the tendons for the feet and toes. Research studies reveal that the flexor digitorum longus muscle is a thin muscle located in the tibia’s deep posterior muscles and provides operational support to the four different sections of the toes and allows flexion. While other research studies reveal that the flexor hallucis longus muscle is a deep posterior muscle located in the fibula and provides flexion to the great toe while serving to plantarflex and inversion to the foot. Now the flexor muscles work together to allow stability to the foot when a person is walking. Additional studies have shown that the flexor muscles are active as many people push off from the heel to allow movement to the toes and feet when stepping on the ground. This action enables the flexor muscles to contract and exerts much energy to allow the feet to move. However, when the body begins to age naturally, or various issues affect the lower body extremities, it can lead to multiple problems affecting a person’s mobility. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Non-radiographic axial spondyloarthritis or nr-axSpA and non-radiographic ankylosing spondylitis/AS are related. However, non-radiographic axial spondyloarthritis can present AS symptoms with active inflammation of the spine and sacroiliac/SI joints, causing back and hip pain but does not reveal joint damage on X-rays or MRIs. Injury Medical Chiropractic and Functional Medicine Clinic can explain what it means to have non-radiographic axial spondyloarthritis, how it can be managed, and what to do to prevent it from turning into ankylosing spondylitis. Non-Radiographic Axial Spondyloarthritis Non-radiographic axial spondyloarthritis means there are early AS symptoms but have not developed enough joint inflammation or damage to show up on an X-ray or other form of imaging. Early evidence of joint inflammation includes blurring of the joint edges and localized regions of joint erosion. It can be difficult for physicians to see these subtle changes on an x-ray. Ankylosing Spondylitis - Ankylosing spondylitis, or AS, is a form of inflammatory arthritis that affects joints in the spine and elsewhere.
- It is a chronic, inflammatory, autoimmune disease.
- Medical research is still ongoing to determine the exact cause, but a genetic component is believed to be contributing factor.
- Around 85% of individuals with ankylosing spondylitis have inherited the HLA-B27 gene, which is associated with multiple autoimmune conditions.
- In the early stages, individuals will present lower back pain around the sacroiliac joints or the joints that connect the spine to the pelvis.
- Later stages have more obvious X-ray findings, like the fusing of the sacroiliac joints and the lower spine that takes place over time.
- Joint inflammation can progress, causing permanent joint damage and spine rigidity.
- Most individuals with the condition can manage their symptoms with NSAIDs, chiropractic care, physical and massage therapy, and range of motion exercises.
Stage 1 - There is no evidence of spinal inflammation on x-rays.
- MRI provides more detailed images of bones and may reveal bone marrow edema or accumulation of fluid in the structures of the spinal bones and joints.
- Individuals with non-radiographic axial spondyloarthritis, you are here.
Stage 2 - There is visible inflammation of the spinal joints on the x-ray.
- The sacroiliac joints between the spine and the pelvis are the most affected.
Stage 3 - Chronic inflammation of the joints has caused bone loss and permanent joint damage, resulting in spine rigidity.
Symptoms of Non-Radiographic Axial Spondyloarthritis There are differences between back pain associated with muscle strain and arthritis. Back pain symptoms include: - Starts to present before age 40.
- It has a gradual onset and can go unnoticed for years.
- Improves with movement or activity.
- Eases up throughout the day.
- Starts up in the evening when resting.
Other symptoms include: - Joint stiffness
- Swollen fingers
- Heel pain
- Bilateral buttock discomfort and pain
Slowing Progression Progression from non-radiographic axial spondyloarthritis to ankylosing spondylitis occurs in 10% - 20% of individuals over a two-year period. Progression factors include genetics, gender, degree of joint damage, and level of inflammatory markers at the time of diagnosis. - Early diagnosis and treatment can slow the progression before significant joint damage with anti-inflammatory therapy, rheumatological therapy, and targeted exercise.
- Work with a specialist like an orthopedic spine specialist and rheumatologist that understands the disorder and is up to date on the most recent treatment modalities.
- A rheumatologist will perform diagnostic tests, including spine X-rays, genetic blood work, and serum inflammatory markers.
- Individuals with non-radiographic axial spondyloarthritis should expect to have serial X-rays to gauge the progression of the disease.
- Staying healthy and active is recommended to slow the progression of nr-AxSpA and AS.
- Recent medical advances and lifestyle adjustments can slow the progression in most cases.
General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.* Our office has reasonably attempted to provide supportive citations and identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please contact Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Six tips for living well with ankylosing spondylitis. Available at https://www.mayoclinic.org/diseases-conditions/ankylosing-spondylitis/in-depth/6-tips-for-living-well-with-ankylosing-spondylitis/art-20478753. Accessed 11/07/2022. Ankylosing spondylitis. Mayo Clinic. Available at https://www.mayoclinic.org/diseases-conditions/ankylosing-spondylitis/symptoms-causes/syc-20354808. Accessed 11/05/2022. D. J. Pradeep, A. Keat, K. Gaffney, Predicting outcome in ankylosing spondylitis, Rheumatology, Volume 47, Issue 7, July 2008, Pages 942–945, https://doi.org/10.1093/rheumatology/ken195 Kucybała, Iwona, et al. "Radiologic approach to axial spondyloarthritis: where are we now and where are we heading?." Rheumatology international vol. 38,10 (2018): 1753-1762. doi:10.1007/s00296-018-4130-1 Michelena, Xabier, López-Medina, Clementina, and Helena Marzo-Ortega. "Non-radiographic versus radiographic axSpA: what's in a name?"." National Center for Biotechnology Information. October 14, 2020. https://doi.org/10.1093/rheumatology/keaa422 Swift D. Ankylosing spondylitis: disease progression varies widely. Medpage Today. Accessed 11/05/2022.Available at https://www.medpagetoday.com/rheumatology/arthritis/49096
Introduction As one of the stabilizers for the body, the knees are located between the thighs and legs, allowing flexion and extension. The knees help the hips by supporting the upper body’s weight and allowing the legs to move from one place to another without feeling pain. The knee has various muscles and ligaments surrounding the knee joint, allowing the leg to be bent when active. One of the muscles is located behind the knee, known as the popliteus, and supports the legs. However, minor injuries or actions can affect the knees causing the joint to be in a “lock” position and develop myofascial trigger points that can induce muscle spasms in the knees. Today’s article focuses on the popliteus muscle, how knee pain is associated with trigger points, and how to manage knee pain through various treatments. We refer patients to certified providers that incorporate multiple methods in the lower body extremities, like knee pain treatments correlating to myofascial trigger points, to aid many people dealing with pain symptoms along the popliteus muscles. We encourage and appreciate each patient by referring them to associated medical providers based on their diagnosis, especially when appropriate. We understand that education is an excellent source to asking our providers intricated questions at the patient’s request. Dr. Alex Jimenez, D.C., only utilizes this information as an educational service. Disclaimer What Is The Popliteus Muscle? Have you been dealing with pain behind your knees? Do you have issues bending your knees when climbing up or down the stairs? Or do your back knee muscles start to twitch uncontrollably, causing muscle spasms? Many knee issues correlate with various factors that can affect the popliteus muscle and develop trigger points. The popliteus is a small muscle with a very important job as it is a major stabilizing muscle to the knees. The popliteus muscle originates from the lateral side of the femur and inserts itself into the posterior surface of the tibia. Some attachments are between the popliteus and lateral meniscus, allowing the knees to be in motion and providing flexion without pain and entrapment. Additional studies reveal that when a person exercises, the popliteus’s basic function helps bring about and maintain internal rotation of the tibia on the femur. The popliteus also helps prevent the foot from external rotation and allows the individual to stand correctly. However, injuries to the knee could overstretch the popliteus muscle and cause mobility issues to the knee flexion. Knee Pain Associated With Trigger Points When dealing with knee pain, it could often be a joint disorder like osteoarthritis or a musculoskeletal condition like sciatica pain associated with the knee. These issues could be due to normal factors like constantly sitting down or bending down to lift heavy objects that cause the knees to buckle. However, when the popliteus muscle has been continuously overused from being bent, it can form tiny nodules known as trigger points to cause knee pain. Studies reveal that trigger points on the muscles surrounding the knee are often ignored during a clinical diagnosis. Trigger points cause referred pain to the surrounding muscles, accompanied by various sensory sensations like heaviness, tingling, and hypersensitivity to the popliteus muscle. In “Myofascial Pain and Dysfunction,” written by Dr. Travell, M.D. stated that one of the chief complaints that many patients often talk to their doctors about is the pain they feel in the back of their knees when they are in a crouch position. The book also states when normal actions like running or twisting have overloaded the popliteus muscle, it can cause trauma or strain to the popliteus muscle and tear the posterior cruciate ligament to the knees. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Introduction The hips and the thighs have an established relationship where mobility and stability play a part in the body’s lower extremities. The lower extremities’ main job is to support the upper body’s weight while stabilizing the hips and allowing movement from the thighs to the legs and feet. When it comes to the thighs in the lower body, the various muscle surrounds the thighs and skeletal joints to allow the legs to move from one place to another. One of the muscle groups in the thighs is known as the quadriceps femoris. This muscle group is activated when a person is in motion and can succumb to injuries from trauma or normal factors. When this happens, issues like myofascial pain syndrome can affect the thigh muscle and cause referred pain to travel to the knees. Today’s article focuses on the quadriceps femoris, how myofascial pain syndrome is associated with thigh pain, and trigger point therapy on the quadriceps. We refer patients to certified providers who incorporate multiple methods in the lower body extremities, like thigh and hip pain treatments correlating to myofascial pain, to aid individuals dealing with pain symptoms along the quadriceps for muscle. We encourage and appreciate patients by referring them to associated medical providers based on their diagnosis, especially when appropriate. We understand that education is an excellent solution to asking our providers complex questions at the patient’s request. Dr. Jimenez, D.C., utilizes this information as an educational service only. Disclaimer What Are The Quadriceps Femoris? Have you been dealing with knee issues when you are walking? What about muscle tenderness or soreness in your thighs? Or have you been experiencing knee complaints when you are running? These areas of complaint are correlated with trigger points associated with thigh pain along the quadriceps femoris. As one of the most voluminous muscles in the human body, the quadriceps femoris is a group of muscles predominant in the thighs and is extraordinarily important. This muscle group is essential for daily activities like climbing the stairs or getting up from a seated position, allowing repercussions on the knees and hip joints. The quadriceps femoris consist of four thigh muscles to allow extension to the knees: - Vatus medialis
- Vatus lateralis
- Vatus intermedius
- Rectus femoris
Studies reveal that these four different muscles fuse to form the quadricep tendon and stabilize the patella and thigh flexion at the hips and knee extension. This muscle group is highly important for athletes participating in sports events but can succumb to injuries through muscle strain. Myofascial Pain Syndrome Associated With Tigh Pain When the thigh muscles, especially the quadriceps femoris, can be overstretched and overused when in motion. Thigh pain is nothing to be alarmed about in its acute form; however, it can develop small nodules along the four muscle fibers that can cause referred pain to the hips and knees. To that point, it can correlate through quadriceps muscle strain to the thighs. Studies reveal that normal factors like kicking, jumping, or a sudden change of direction of running can potentially cause the muscle fibers to be overstretched and develop pain due to localized swelling corresponding to loss of motion from myofascial pain syndrome. In “Myofascial Pain and Dysfunction,” written by Dr. Janet G. Travell, M.D., the book states that myofascial pain syndrome can invoke referred pain to the affected muscle or muscle group, causing the body to be dysfunctional. Myofascial pain syndrome associated with thigh pain can be managed through various treatments and could allow mobility back to the thighs, legs, knees, and hips. The book even mentions how the four muscles in the quadriceps femoris cause different pain issues in various body parts due to myofascial pain syndrome. For the rectus femoris, many people would complain about knee pain and weakness when climbing stairs. The vatus medialis would initially produce a toothache-like pain deep within the knee joint, often misinterpreted as joint inflammation. The vatus intermedius causes many individuals to have difficulty fully straightening their knees and causes them to develop buckling knee syndrome. And finally, the vatus lateralis could cause many individuals to complain about feeling pain when walking and that the pain is being distributed on the lateral aspect of the thigh, including the knees. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Introduction The lower body extremities help provide stability to the various body parts, including the hips, thighs, pelvis, legs, knees, and feet. The hips and thighs comprise multiple muscles and nerves that provide mobility to the lower half and allow the host to move around in different locations. While the hip muscles act on the thigh muscles at the hip joint and stabilize the pelvis, the thigh muscles allow the lower body to bend, flex and rotate while bearing most of the upper body’s weight and keeping alignment with the hips and legs. One of the thigh muscles is the sartorius muscle, and if it becomes overused and injured can lead to complications in the form of myofascial pain syndrome. Today’s article post examines the sartorius muscle, how myofascial trigger pain is associated with the sartorius, and the effectiveness of myofascial pain treatment on the thighs. We refer patients to certified providers who incorporate multiple methods in the lower body extremities, like thigh pain treatments correlating to myofascial pain syndrome, to aid individuals dealing with pain symptoms along the sartorius muscle. We encourage and appreciate patients by referring them to associated medical providers based on their diagnosis, especially when appropriate. We understand that education is an excellent solution to asking our providers complex questions at the patient’s request. Dr. Jimenez, D.C., utilizes this information as an educational service only. Disclaimer What Is The Sartorius Muscle? Are you experiencing pain in the upper, mid, or lower parts of your thighs? Do you have difficulty walking for long periods? Or do your knees hurt more than usual? Most of these issues correlate with myofascial trigger pain associated with the sartorius muscle. As the longest muscle that spans from the hips to the knee joints, the sartorius muscle, or the “tailor muscle,” serves as both a hip and knee flexor while working with other muscles that allow hip mobility. The sartorius shares its origin location with the TFL (tensor fascia latae) muscle at the anterior superior iliac spine and is responsible for internal rotation at the hips. In the book, “Myofascial Pain and Dysfunction,” the author Dr. Janet G. Travell, M.D., mentioned that the sartorius muscle assists the iliacus and the TFL muscles in hip flexion while assisting the short head of the bicep femoris in the knees for knee flexion, allowing the individual to walk for long distances. Even though this long muscle assists in hip and knee flexion, it can succumb to injuries and create issues with the hips and knees in the lower body. Myofascial Trigger Pain Associated With The Sartorius Muscle When traumatic forces or normal factors begin to affect the sartorius muscle, the surrounding muscles on the thighs and hips are also affected. The sartorius muscle allows the individual to move around and allows flexion to the hips and knees when injuries or the muscle is being overused; it can cause pain-like symptoms that correlate with hip and knee issues associated with myofascial trigger pain. Myofascial trigger pain along the sartorius muscle doesn’t usually occur in the muscle but can occur in conjunction with trigger point involvement in the surrounding muscles. Studies reveal that myofascial trigger pain is found in the hip muscles and can cause issues in the lumbopelvic-hip muscles of the lower body. This causes referred pain on the sartorius to be more diffused and superficial to the knees. When myofascial trigger pain is associated with the sartorius, many individuals often mistake it for knee pain. To that point, myofascial trigger pain could affect how a person walks and bends at the knees. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Introduction The upper body works because it provides stability for the body and motor-sensory functions to the arms, neck, shoulders, and chest. The muscles surrounding each body section have different roles and outputs that have specific jobs for body functionality. For the chest body area, the various muscles are there to support the shoulders and arms while protecting the chest cavity and the internal organs inside. Some of the different chest muscles even support the internal organs and the rest of the muscles. One of those muscles is known as the serratus anterior muscle. Today’s article looks at this muscle, how trigger points affect the serratus anterior muscle, and various actions to manage trigger points along the serratus anterior. We refer patients to certified providers who provide different techniques in pain therapies associated with trigger points to aid many suffering from pain-like symptoms along the serratus anterior muscle along the ribcage. We encourage patients by referring them to our associated medical providers based on their examination when it is appropriate. We designate that education is a great solution to asking our providers profound and complex questions at the patient’s request. Dr. Alex Jimenez, D.C., notes this information as an educational service only. Disclaimer What Is The Serratus Anterior? Have you been experiencing pain in your sides? Do you notice that your shoulders feel stiff when rotating backward? Or are you experiencing any cardiovascular disorders that are causing you pain? Pain can come in many forms and affect a person differently, as most of these symptoms are associated with trigger points affecting the serratus anterior muscle along the side of the ribs. The serratus anterior muscles work in the body because this muscle is located deep within the scapula (shoulder blades) and the pectoral muscles. Some of the functions that the serratus anterior provides are that it helps pull the shoulder blades forward around the thorax by allowing anteversion and protraction of the arms. A great example is when a boxer is throwing a punch. This motor action is done with the long thoracic nerve. The long thoracic nerve originated from the C-5 and C-6 regions of the cervical spine and is the motor nerve for the serratus anterior muscle to allow an anterolateral motion for the shoulder blades that allows arm elevation. Another function of the serratus anterior is that it helps lift the ribs and provide assistance with respiration. The serratus anterior muscle also helps protect the side of the ribcage. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
|



 Your new post is loading...
Your new post is loading...









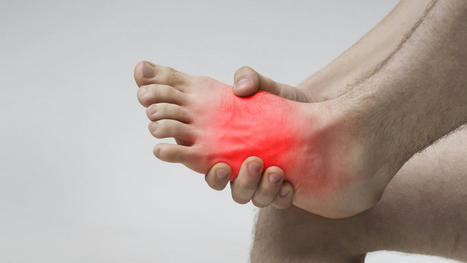

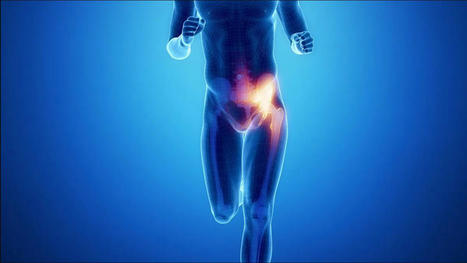

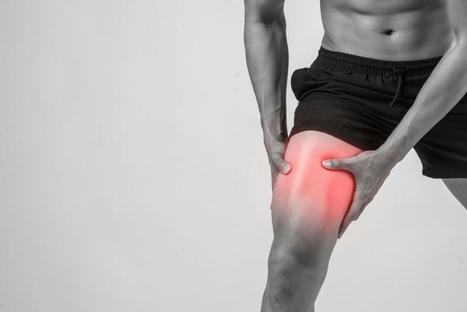


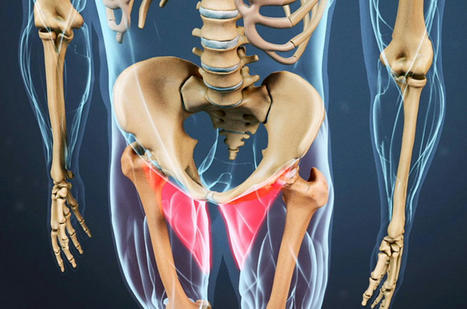











Dr. Alex Jimenez gives an insight look at how many people uses biomechanical self-help methods using the MET technique. If you have any questions or concerns, please call Dr. Jimenez at 915-850-0900.